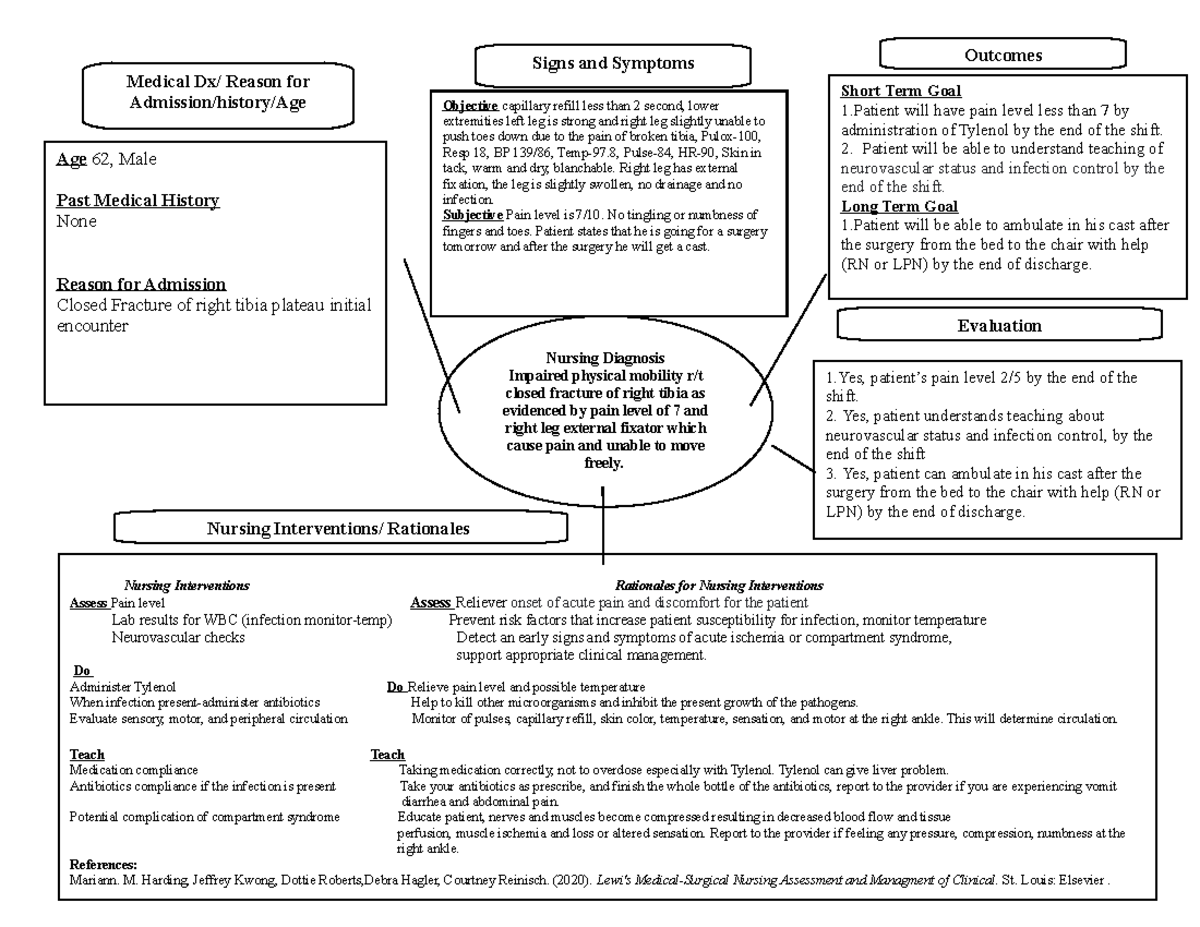
after hemiarthroplasty, mobilisation may start earlier, while following extracapsular fracture, it may be delayed. Mobilisation strategy, type of weight bearing, timing and progress of exercise depend on the type of fracture and surgery and there are contradictions about evidence-based pathways for management after different fractures and procedures e.g. Patients who were mobile before the fracture should be mobilised regardless of their cognitive status and the focus should be on gait quality, walking endurance, activities of daily living and safety.

It is essential to consider the impact of these multiple factors on exercise and mobility and take an individualised, holistic approach. The main factors that impact on ability to remobilise are summarised in Box 6.1. 9), which are also associated with poorer mobility outcomes and limit participation in exercise. Other conditions to consider include depression, cognitive impairment and delirium (Chap. Frailty leads to poor outcomes and affects capacity for mobilisation and exercise.
For every day spent in bed, 2.5 days are needed to regain the strength to walk. The progressive loss of muscle mass with ageing is associated with decreasing reserves and sarcopenia (Chap. There are numerous factors that affect ability to remobilise. Management of the fear of falling is also central, along with the need to educate patients and carers about fall prevention and the importance of exercise. Those who are not remobilised early may feel demoralised, so it is important that they have realistic expectations to avoid disappointment.
Older women have been found to prefer being dead than experience loss of independence, demonstrating the psychological impact. Patients also suffer from loss of confidence, fear of falling and are at risk of further fractures and other complications. Good pain management helps avoid delays in rehabilitation, postoperative complications, delayed discharge and unsafe mobility. Muscle strength deficit in the fractured limb is associated with even greater pain and it is unethical to expect patients to comply with rehabilitation exercises without managing pain effectively. Pain limits remobilisation and is associated with delirium, depression, sleep disturbances and poor mobility. For older people following hip fracture, early mobilisation is especially important because it is linked to mortality and functional recovery as well as risk of functional decline due to the injury, perioperative immobilisation, muscle weakness, fatigue and postoperative complications. Mobilisation is essential for health-related quality of life and independence. The aim of this chapter is to highlight the risks of immobility and the benefits of remobilisation and exercise to enable clinicians to effectively manage the multiple and interconnected individual factors of each patient to maximise their function. Patients should undergo multidisciplinary assessment to identify factors known to be associated with risk for poor functional recovery so that appropriate multidisciplinary interventions can be implemented. Many patients never recover their previous level of function after a fragility fracture and there is significant risk of institutionalisation, new fractures, disability and loss of independence. Recovery is often compromised for those with limited pre-fracture activity and cognitive impairment, low functional levels postoperatively, older age, polypharmacy, comorbidities, depression, poor nutritional status, lack of social support and not living independently. Individual patient goals are determined by their pre-fracture mobility and functional status. A central goal of nursing care following fragility fracture is to maximise mobility. Being mobile and able to self-care and fear of falling are important to patients. The positive effects of physical activity on physical and mental health are well known and include weight control, improved balance, flexibility, strength, anxiety reduction and protection from ill health, as well as contributing to independent living and preventing falls.
